This week, Immersed is thrilled to bring you a guest blog post on the human microbiome by Dr. Anne M. Estes, a postdoctoral fellow at the Institute for Genome Sciences at the University of Maryland, School of Medicine in Baltimore.
You are NOT Human!
When you look in the mirror, what you do not see is extremely important for your health. Meet your microbiome—all the bacteria, fungi, and viruses living in and on you [1]. While scientists are unsure exactly how many microbial cells are present in and on humans, we currently estimate that there are at least three times more and perhaps ten or one hundred times the number of microbial cells than human cells [2]. Hey—wait—back away from the hand sanitizer! The vast majority of these microbes are helpful. We’ve been brought up to think of viruses and bacteria strictly as “germs” that cause disease, but without helpful microbes you wouldn’t be able to properly digest your food [3] and would lack certain vitamins [4–6]. In fact, it’s the loss of these helpful microbes that corresponds with an increase in several diseases including diabetes, allergies, asthma, obesity, autism, and numerous digestive system disorders such as irritable bowel syndrome, colitis, Crohn disease, and celiac disease. The symptoms with each of these diseases is different. However, the National Institutes of Health–funded Human Microbiome Project (HMP) and other projects have discovered that people with each of these ailments have a microbiome that is strikingly different from that of healthy people [7–11]. This information about the human microbiome is changing the way both basic science and medicine think about human health [12].
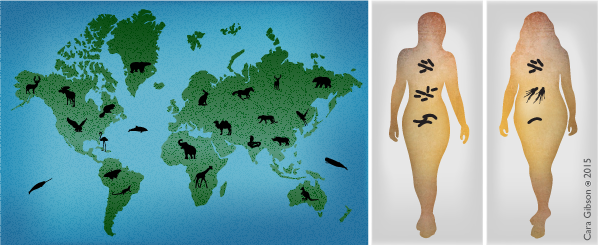
Left: Diversity of animals living in different habitats of the Earth. Right: Different bacteria found on individual people.
You are a Planet!
You are a home for trillions of microbial cells [13–16]. A walking, talking, microbial planet. The bacterial component of the microbiome is best understood. Bacteria are so tiny that millions of them can fit on the antennae of an ant. The ratio of the size of the common gut bacterium Escherichia coli (E. coli) compared to your body is similar to the ratio of a human body compared to the Earth. Just like the Earth has different habitats–mountains, lakes, deserts, swamps–so does the human body. In each of the Earth and human habitats, specific organisms flourish in those particular conditions. Different bacteria, fungi, and viruses live in the rainforest-like habitat of your armpit than live in the hot, dry, low nutrient, and high UV intensive desert-like habitat of the back of your hand. The HMP set out to map out some of the bacterial habitats of the human body. To visualize these different communities, the HMP made a neat interactive program called SitePainter that maps where a certain bacterium is found on the body [17]. Try it out and see which bacteria are found in various locations. As you switch between bacterial types, you’ll see how many or few places they can live. You may also notice microhabitats within larger habitats. In the mouth, some bacteria are only found in a portion of the plaque near the tooth surface. Others, only in the dry skin behind the ear.
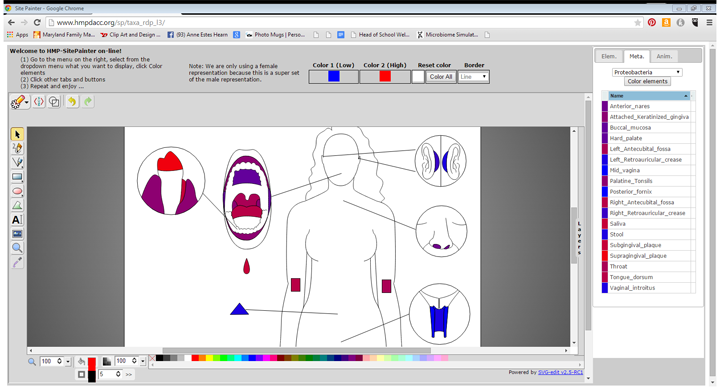
An Image captured from SitePainter demonstrating the different habitats where various bacteria are found.
Create your own map at http://www.hmpdacc.org/sp/.
Take a minute to imagine how many different bacterial habitats are on and in you. How do you think the temperature, moisture, and nutrients in your bellybutton compare to your nostril? Stomach? Mouth? Front teeth versus molars? Each different mixture of these physical parameters potentially creates a new habitat. Add in the amount of oxygen, pH, and osmolarity of the body habitat as well and you can quickly think about the vast diversity of bacterial habitats your body has, especially for microscopic organisms. I doubt anyone has calculated a specific number of body habitat sites and that number doesn’t really matter. What is important is that when considered from a microscopic organism’s perspective, in and on your body are a vast array of potential places to live. How these microbes get to the particular habitat and survive and how they are restricted from other habitats is under study.
What you DO with that body and what you feed your body will also change the habitat for your bacterial residents. Do you bathe daily? Weekly? Do you use antibiotic soaps? Play in the dirt? the ocean? your room? Do you have a dog? Cat? Gerbil? Baby sister? How were you born? What were you fed as an infant? All of these factors can change your resident microbiome. Harsh cleaners and antibiotics can damage your natural microbiome. Where you play and what you play with may introduce new microbes from the environment to your residential microbiome if there are open spaces for the bacteria to live in and the proper conditions for them to survive.
You Never Dine Alone
You’re colonized with trillions of bacteria. So what? These invisible inhabitants of Planet You are quite important. Sometimes they are breaking down nutrients or toxins, sometimes they make vitamins, other times they simply take up a space and prevent a pathogen from living there. In many cases, scientists are just beginning to understand what’s going on and new features are frequently discovered. In some cases, these bacteria are working together with other bacteria or other microbes to feed off of one another. In the macro-ecosystems of Planet Earth, plants use carbon dioxide that animals exhale and the sun’s energy to make sugars to help themselves grow. Plants “exhale” oxygen as a waste product of this sugar making process (called photosynthesis). Animals can then use the oxygen and plant sugars, as well as animal proteins, to help themselves grow. Plants and animals feed off of and recycle each other’s waste products. Without oxygen from photosynthesis, animals would not live. The ecosystem would collapse.
Similarly, microbes use each other’s waste products to grow. One microbe’s waste products are another microbe’s dinner. Particular microbes have distinct sets of genes that allow those microbes to break down specific nutrients from what the host eats. For example, some digestive system bacteria feed on plant fibers. If their human host doesn’t eat any or very little complex plant fibers, the bacteria will not get fed. Some of these bacterial types may turn to feeding on the protective mucus the large intestine produces and creates problems for the host [18]. Others may enter a dormant stage waiting for the food they can eat. Other bacteria synthesize vitamins such as the B vitamins and vitamin K. Without those vitamins, the human host can have a range of problems from decreased blood clotting to immune and nervous system problems [19].
You Microbial Planet, You
From head to toes, inside and out, you are a planet for your resident microbes. Though these microbes are invisible to the naked eye, their importance is becoming increasingly apparent. As Earth has a series of habitats with characteristic organisms, so does the human body. Without the many microbes that call you home, your ecosystem can malfunction. Diet is one of the key ways to take care of your microbiome. A future post here will discuss what is currently known about the influence of diet on the gut microbiome. For more information on the interaction between microbes and human health, see my blog Mostly Microbes. It is my hope that my blog will serve to connect you to this invisible and essential part of yourself.
REFERENCES
- Lederberg, J., and A. McCray. 2001. Ome sweet ‘omics:—A genealogical treasury of words, p. 8. The Scientist, vol. 15.
- The Human Microbiome Project Consortium. 2012. Structure, function and diversity of the healthy human microbiome. Nature 486:207–214.
- Cantarel, B. L., V. Lombard, and B. Henrissat. 2012. Complex carbohydrate utilization by the healthy human microbiome. PLoS ONE 7:e28742.
- LeBlanc, J. G., C. Milani, G. S. de Giori, F. Sesma, D. van Sinderen, and M. Ventura. 2013. Bacteria as vitamin suppliers to their host: a gut microbiota perspective. Current Opinion in Biotechnology 24:160–168.
- Hausmann, K. 1955. The significance of intestinal bacteria for vitamin B12 and folic acid supply in humans and animals. Klin Wochenschr 33:354–9.
- Albert, M. J., V. I. Mathan, and S. J. Baker. 1980. Vitamin B12 synthesis by human small intestinal bacteria. Nature 283:781-2.
- Cho, I., and M. J. Blaser. 2012. The human microbiome: at the interface of health and disease. Nat Rev Genet 13:260-270.
- Hofer, U. 2014. Microbiome: Bacterial imbalance in Crohn’s disease. Nat Rev Micro 12:312–313.
- Turnbaugh, P., M. Hamady, T. Yatsunenko, B. Cantarel, A. Duncan, R. Ley, M. Sogin, W. Jones, B. Roe, J. Affourtit, et al. 2009. A core gut microbiome in obese and lean twins. Nature 457:480–484.
- Ley, R., P. Turnbaugh, S. Klein, and J. Gordon. 2006. Microbial ecology: human gut microbes associated with obesity. Nature 444:1022–1023.
- Qin, J., Y. Li, Z. Cai, S. Li, J. Zhu, F. Zhang, S. Liang, W. Zhang, Y. Guan, D. Shen, et al. 2012. A metagenome-wide association study of gut microbiota in type 2 diabetes. Nature 490:55–60.
- Khanna, S., and P. K. Tosh. 2014. A clinician’s primer on the role of the microbiome in human health and disease. Mayo Clinic Proceedings 89:107–114.
- Costello, E. K., K. Stagaman, L. Dethlefsen, B. J. M. Bohannan, and D. A. Relman. 2012. The Application of Ecological Theory Toward an Understanding of the Human Microbiome. Science 336:1255–1262.
- Zhou, Y., H. Gao, K. Mihindukulasuriya, P. La Rosa, K. Wylie, T. Vishnivetskaya, M. Podar, B. Warner, P. Tarr, D. Nelson, et al. 2013. Biogeography of the ecosystems of the healthy human body. Genome Biology 14:R1.
- Pepper, J. W., and S. Rosenfeld. 2012. The emerging medical ecology of the human gut microbiome. Trends in Ecology & Evolution 27:381–384.
- Turnbaugh, P., R. Ley, M. Hamady, C. Fraser-Liggett, R. Knight, and J. Gordon. 2007. The human microbiome project. Nature 449:804–810.
- Gonzalez, A., J. Stombaugh, C. L. Lauber, N. Fierer, and R. Knight. 2012. SitePainter: a tool for exploring biogeographical patterns. Bioinformatics 28:436–8.
- Johansson, M. E., J. K. Gustafsson, J. Holmen-Larsson, K. S. Jabbar, L. Xia, H. Xu, F. K. Ghishan, F. A. Carvalho, A. T. Gewirtz, H. Sjovall, et al. 2014. Bacteria penetrate the normally impenetrable inner colon mucus layer in both murine colitis models and patients with ulcerative colitis. Gut 63:281–91.
- Kau, A. L., P. P. Ahern, N. W. Griffin, A. L. Goodman, and J. I. Gordon. 2011. Human nutrition, the gut microbiome, and immune system: envisioning the future. Nature 474:327–336.
About Anne:

Dr. Anne Estes.
Dr. Anne M. Estes currently does research on dung beetle microbiomes as a post-doctoral fellow at the Institute for Genome Sciences at the University of Maryland, School of Medicine in Baltimore. Anne is also known as “mama” by two curious and fun little ladies, ages 2 and 7. Though her blog, Mostly Microbes, Anne explores the interactions between microbes and their human hosts. She focuses on the importance of the human microbiome for and during pregnancy, birth, infancy, and early childhood. Microbiology themed kids and adult books, education tools, games, and resources are also featured on Mostly Microbes.